A Guide on Understanding the Techniques of Cataract Surgery
Cataracts are a leading cause of visual impairment and blindness worldwide, far from a mere inconvenience to the millions of people affected. But cataract surgery can significantly improve their quality of life.
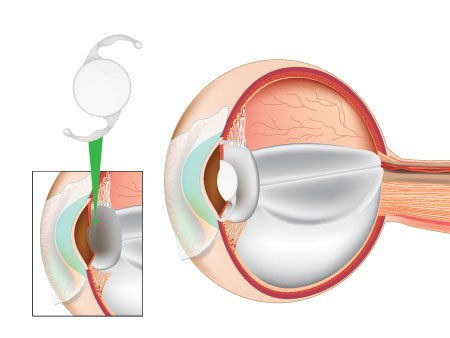
The surgeon makes a small incision and then uses ultrasound to break up the cataract into fine particles, which are then washed out with water. Finally, an artificial lens (otherwise known as an intraocular lens, or IOL) is inserted. In most cases, the wound leaves itself unstitched.
Intracapsular Extraction
Your doctor will suggest this procedure in you, for example, when your cataracts are so dense that you can no longer see clearly with them. In this method, the surgeon makes a large incision to excise your lens and the front capsule of your eye that keeps your lens in place. One difference from the phacoemulsification is that this procedure requires sutures to be placed to close the incision.
This procedure, which was once more common, carries a risk of complications, such as posterior capsular opacification (PCO) that can lead to retinal detachment.
To perform this surgery, your doctor coats the entire surface of the eye with liquid nitrogen to freeze certain fibres that secure the cataract in the lens capsule, then your doctor uses a needle to poke a hole in the cornea before pulling your natural lens out of your eye and replacing it with an artificial one. Your doctor can also opt to put a different type of intraocular lens inside you. Depending on your needs, you might need a multifocal or aspheric lens to correct short-sighted vision (myopia), long-sighted vision (hyperopia), and/or astigmatism.
Extracapsular Extraction
The aim of modern cataract surgery is to replace a clouded, natural lens with an implanted clear artificial plastic lens. There are two methods for doing this – phacoemulsification and extracapsular extraction (ECCE).
This procedure involves your ophthalmologist (doctor who specialises in eyes and the eye) viewing your living eye through a microscope on a table to make micro incisions (cuts, with either a blade or laser) at the edge of your cornea and then breaking up the cataract with a small instrument of some kind and removing it, through suction, from your eye.
However, it requires a larger incision and takes a longer time to heal than phacoemulsification. Because modern procedures are more advanced, phacoemulsification has become the predominant type of cataract removal in the US, but ECCE remains commonly used in much of the world, where phaco equipment is impractical. Dr Ulrich performs monthly free cataract surgeries in Mexico as part of the Flying Samaritans. ‘I think the ECCE makes more sense there, because it’s cheaper than phaco,’ he says.
Phacoemulsification
Phacoemulsification uses ultrasonic energy to break your cataract into pieces, which are then aspirated away using suction, while an intraocular lens implant (IOL) made from either silicone or acrylic is placed into the same capsule that once held your natural lens.
During this part of the process, your eye surgeon will deliver high-frequency ultrasonic energy to the eye using a handheld device called a phaco handpiece. The phaco handpiece vibrates at a high frequency causing the cataract to emulsify, or turn into a fluid-like gel. At the same time, as the phaco handpiece emulsifies the cataract, it also continuously aspirates any fluidised anatomical material to maintain a clear surgical field.
The speed and volume of the aspiration flow are important to the efficiency and safety of cataract surgery. To prevent a condition such as Bell’s phenomenon – in which the anterior chamber becomes less pressurised and the eye involuntary opens wide – the aspiration speed should be controlled such that it is proportional to the fluid entering and leaving the eye.
Laser Extraction
Your ophthalmologist cuts a little hole in the eyeball, then fragments the cataract with a little bulb at the end of a suction tube that sucks out the pieces. He puts in a plastic, silicone or acrylic artificial lens, and sews it up.
Your vision should be clear within one or two days of surgery. You’ll want to stay quietly and avoid strenuous activity, but your health care practitioner will advise you when it’s okay to go back to work and other activities.
In three of 10, you might develop a clouding of the back part of the capsular bag (the tissue that nests the lens inside the eye) called posterior capsular opacification (PCO). Again, this problem is not related to the surgery but to the growth of advanced scar tissue in the lens capsule (the silky bag that nests the lens in the eye). PCO is easily corrected in five minutes with a technique called YAG laser capsulotomy. It’s painless and restores vision. Your doctor can do that in the office. It’s less costly than phacoemulsification.


